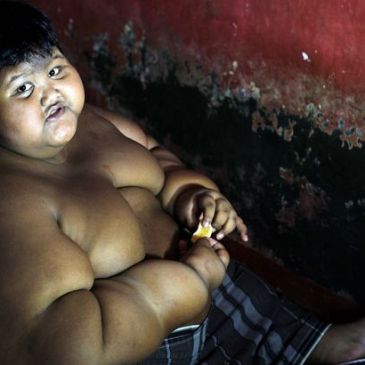
Triple Burden What? Talk About Micronutrient Deficiencies
If you thought double burden of malnutrition (coexistence of undernutrition and obesity) was bad, there is even a Triple Burden. Triple burden of malnutrition is the coexistence of three diseases: undernutrition, micronutrient deficiency and obesity. Micronutrient deficiency is also referred as ‘hidden hunger’ which is the lack of vitamins and minerals.
Compared with the other two diseases, micronutrient deficiency does not necessarily have to be visible from the outside. Undernutrition and micronutrient deficiency together is a problem which often affects individuals, but micronutrient deficiency and obesity is a combination that occurs as well. This happens when an individual eats too many calories a day, but not the right minerals, vitamins etc. The intertwining of all three of these contribute to the triple burden. This burden can be traced back to poverty, a lack of access to adequate diet, poor infant feeding practices, and the sales of unhealthy and cheap processed foods that combined, all lead to undernutrition, micronutrient deficiency, and overweight and obesity!
There are different symptoms micronutrient deficiency, because there are different micronutrients. Deficiency in iron for example, can cause fatigue, weakness, headaches, and pale skin. It can even cause cravings to items which isn’t food, like clay. Another example of micronutrient deficiency is calcium deficiency. Symptoms are weak hair and nails, memory loss, and seizures. The list is long of the different micronutrient deficiencies and I could go on forever, but the picture is clear that micronutrients are important. So eat your veggies kids.
 Maybe you noticed, but besides the symptoms of micronutrient deficiencies that may not be very pleasant, they also can vary. So there are not really distinctive symptoms that says “You have a micronutrient deficiency.” For instance in some studies they used mid-upper-arm circumference to detect nutrient deficiency. The smaller the mid-upper-arm circumference, the greater the chance of having a micronutrient deficiency. But think about this– For the combination undernutrition and micronutrient deficiency, this would be a good method, but for the combination of obesity with micronutrient deficiency, this would not work. And also for people with a normal BMI (and thereby normal mid-upper-arm circumference) this method would not be suitable.
Maybe you noticed, but besides the symptoms of micronutrient deficiencies that may not be very pleasant, they also can vary. So there are not really distinctive symptoms that says “You have a micronutrient deficiency.” For instance in some studies they used mid-upper-arm circumference to detect nutrient deficiency. The smaller the mid-upper-arm circumference, the greater the chance of having a micronutrient deficiency. But think about this– For the combination undernutrition and micronutrient deficiency, this would be a good method, but for the combination of obesity with micronutrient deficiency, this would not work. And also for people with a normal BMI (and thereby normal mid-upper-arm circumference) this method would not be suitable.
Anyways, going back to Indonesia. A lot of children (and adults) are undernourished and also have a micronutrient deficiency, however, obesity is also a problem that occurs additionally. Therefore, the triple burden of malnutrition is present in Indonesia!
So by tackling the problem undernourishment, strategies should also take the micronutrient deficiency in consideration, as well as the problem of obesity in Indonesia. The Australian government actually helped to use strategies to combat undernutrition and micronutrient deficiency for Indonesia. The Australian government did not try to just provide food, but also made up for the micronutrient deficiency. However, they did not take into consideration the problem of obesity when implementing the interventions. What can be a good way to implement all three problems into one intervention? Is it possible?
Fun fact: Did you know you could have micronutrient deficiency which is not food related?
A micronutrient deficiency of vitamin D. You get this vitamin of the sun, but if an individual does not get in a lot of contact with the sun, he or she can not get this vitamin. In Indonesia this problem occur, especially with women. This is because they cover up a lot of there body for their religion.
Written by: Una
The Faces of Malnutrition. (2016, July 20). Retrieved December 1, 2016, from https://www.unicef.org/nutrition/index_faces-of-malnutrition.html

 Malnutrition can affect all areas of health and be detrimental to daily activities. The insidious nature of malnourishment is that eating either too much or too little causes this issue. How can you make sure you’re eating properly?
Malnutrition can affect all areas of health and be detrimental to daily activities. The insidious nature of malnourishment is that eating either too much or too little causes this issue. How can you make sure you’re eating properly?




 How is the double burden of malnutrition even possible? Undernourishment is understandable. Lack of money and poverty can lead to the lack of food and thereby undernourishment. But somehow a country who deals with this poverty problem, also has to deal with obesity, which can imply that people are consuming too much food or more specifically, an overconsumption of sugary and fatty foods.
How is the double burden of malnutrition even possible? Undernourishment is understandable. Lack of money and poverty can lead to the lack of food and thereby undernourishment. But somehow a country who deals with this poverty problem, also has to deal with obesity, which can imply that people are consuming too much food or more specifically, an overconsumption of sugary and fatty foods.